
Explaining Near-Record Health Spending Growth during the 2020 Decline in Health Care Utilization
Introduction
Recently released data from the Centers for Medicare & Medicaid Services (CMS) summarized in Health Affairs show that spending on health care in the first year of the COVID-19 pandemic increased 9.7% from the prior year, reaching a record total of $4.1 trillion dollars. Surprisingly, this increase in health care spending came during a period of declines in utilization of most health care services, including less hospital care, fewer outpatient visits, declines in nursing home and residential care residents, and fewer dental visits, largely due to the postponement of elective care, delay in treating other health needs, and general avoidance of in-person visits during the pandemic. Compensating for the decline in utilization and revenues from patient care in 2020 were large increases in direct, lump-sum government support for the health care industry, including Paycheck Protection Program (PPP) loans, CARES Act Provider Relief Funds, and other government assistance programs. In this blog, we assess the overall impact of federal health care system support on the 2020 health spending estimates, decompose the total government support across different health sectors using the new CMS data, and estimate the distribution of 2020 health spending by month with and without the federal government assistance.
Methods
Data describing national health expenditures in 2020 were taken from CMS’ detailed “National Health Expenditures by type of service and source of funds” spreadsheet, whose contents are described in the Health Affairs paper. We used our Health Sector Economic Indicators methodology to distribute these expenditures across months with and without the increased lump-sum federal expenditures in response to the COVID-19 pandemic. We estimated the magnitude of these increased federal expenditures to be the amount by which 2020 federal spending on the CMS categories of “Other Federal Programs” and “Public Health Activity” exceeded the amount spent in 2019. (Our numbers therefore disagree slightly with those presented in Health Affairs, which describes the total amounts spent in these categories in 2020.) We assumed that the increase in federal spending began in May (most government spending in response to the pandemic became available in April but ramped up in subsequent months) and was spent uniformly across all months from May through December.
Overall Impact of COVID-Specific Effects
Increases in federal government spending having the most impact on health spending growth in 2020 included funds given to health care providers to assist with COVID-related lost revenue and increased costs, and increased funding for federal public health initiatives for development of COVID-19 vaccines and treatments, stockpiling of vaccines and drugs, and preparedness. These spending increases were not directly related to patient care, helping to explain the apparent paradoxical large increase in expenditures that accompanied the decline in utilization of many health care services.

Exhibit 1 shows the impact of these increases on national health spending and on the spending components that received this government support, which included $179.9 billion dollars allocated to providers and an increase of $114.9 billion for public health activities, for a total contribution of $294.8 billion. As CMS notes, without this federal spending, year-over-year growth in health care costs would have been 1.9% rather than 9.7%. The rightmost columns in Exhibit 1 display the growth with and without the federal spending increase for each spending category. With the additional federal spending, none of these spending categories except dental services experienced a decline in spending in 2020; without them, spending on hospital care, physician and clinical services, and other professional services would have declined. The increase in federal spending on government public health activities caused this spending to be more than double the amount spent without the increase.
Exhibit 1. Impacts of Federal Government Spending Increases on National Health Spending in 2020 (millions of dollars)
Other increases in federal spending, not shown in the exhibit, supported patient care more directly. Most notable among them was an 18.8% year-over-year increase in federal Medicaid expenditures― $72.7 billion more than was spent in 2019. This increase was due to both a 5.1 percent increase in Medicaid enrollment in 2020 and the 6.2 percentage point increase in the federal medical assistance percentage (FMAP) that was effective beginning January 1, 2020 and will continue through the quarter in which the COVID-19 public health emergency declaration is terminated.
A COVID-related contribution to the growth in spending in 2020 that was not directly caused by increased federal spending was a significant increase in the net cost of insurance, which grew by 27.4% to $301.4 billion. There are two main factors contributing to this increase. First, the Affordable Care Act (ACA) Health Insurance Tax (HIT), which was suspended from 2017 through 2019, took effect again in 2020. It was repealed permanently starting in 2021, but the IRS estimated the HIT for 2020 at $15.5 billion, a significant share of the $21.6 billion increase in the net cost of private health insurance between 2019 and 2020. The second factor was a larger than usual gap between premium revenues and health care outlays due to reduced health care utilization under the pandemic. The ACA’s medical loss ratio (MLR) restrictions reduced this gap by requiring rebates from many commercial insurers in 2020, but more plans likely reached the MLR limits and not all plans are subject to the ACA’s rebate requirements. The gap between dollars taken in and health care outlays for 2020 was also larger for private sector managed care plans covering beneficiaries under both the Medicare and Medicaid programs, as net cost of insurance increased under both public programs as well.
Detailed Impacts of Increased Federal Government Spending
We estimated monthly spending growth in 2020 for total national health spending and each of the six categories of spending on health care services with the largest increases in government spending that were summarized in Exhibit 1. The graphs in Exhibit 2 show the cumulative rates of growth in spending from January 2020 through the end of the year with and without the non-patient-care increases in federal spending.
Exhibit 2. Cumulative Spending Growth Since January 2020, by Major Category
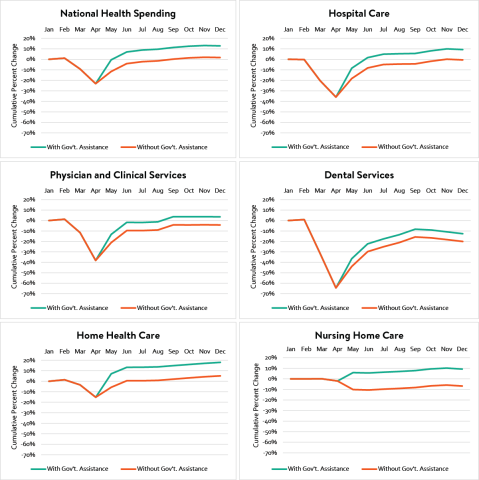
The federal government assistance helped ensure positive spending growth for hospital care, physician and clinical services, and nursing home care. Nursing homes in particular benefited from the federal spending and would have sustained a significant decline in revenues without the federal assistance. (The qualitatively different pattern of spending growth for nursing homes compared with the other components was driven by the fact that the large decline in nursing home spending occurred one month later than for the other components, in May rather than April.) Federal assistance also represented a substantive share of 2020 spending on home health care (7.9%), although this sector achieved positive spending growth by mid-2020 even without the additional federal dollars. On the other hand, the federal assistance to the dental sector, while a comparable share of 2020 expenditures (6.1%) to hospitals (6.7%) and physician and clinical services (5.4%), was not enough to offset the dramatic decline in spending on dental services early in the pandemic, making dental services the one major sector with negative spending growth at the end of 2020 even with the additional funding.
Summary
The large year-over-year increase in national health expenditures in 2020 in the face of lower utilization of health care services is largely explained by an increase in federal government spending of $294.8 billion that was not directly tied to the provision of health care services. This increased spending provided essential funds to federal public health activities that led to the development and stockpiling of COVID-19 vaccines and therapeutics. It also provided major support to struggling providers facing declining demand and increasing costs related to the pandemic.
We have incorporated these effects into our Health Sector Economic Indicators methodology and have developed preliminary estimates of health care expenditures through October 2021. These estimates reflect the expectation that elevated spending on public health and federal financial support to health care providers has continued in 2021. While there is significant uncertainty in the 2021 estimates, they provide an initial look at likely spending patterns as we continue to battle the pandemic.
The authors would like to thank the Robert Wood Johnson Foundation for their support of this study and Altarum’s health sector tracking and research. Opinions and findings expressed herein are solely those of the report authors.